Electronic Health Records (EHRs) are no longer optional; they are the backbone of every modern healthcare practice. According to recent industry research, over 80% of US healthcare providers agree that organized data retention in EHRs significantly improves clinical decision-making and patient outcomes. A robust EHR system doesn’t just store information; it automates workflows, improves efficiency, and reduces errors in medical billing and revenue cycle management (RCM).
However, not all EHR systems are created equal. A poorly designed system or a rushed EHR migration can lead to billing errors, delayed claims, and revenue loss. If you’ve noticed workflow inefficiencies, frequent claim denials, or frustrated staff, it may be time to consider switching your EHR system. Similarly, if your vendor is sunsetting your software, this is an ideal opportunity to upgrade to a modern system that aligns with your practice’s needs.
This guide explains how US healthcare providers can switch EHR systems without disrupting billing, minimizing RCM risks, and ensuring a smooth, compliant transition in 2026.
Why Switching EHR Systems Poses Financial and Operational Risks
Switching your electronic health record (EHR) system is not just a technology upgrade; it’s a high-stakes financial and operational decision for any healthcare practice, especially when considering its direct impact on medical billing services and overall revenue cycle performance. While a new system promises improved workflows and better patient care, the transition itself can introduce serious risks if not carefully planned.
Research shows that 15-20% of medical claims are denied on first submission. During an EHR migration, this rate can rise significantly if billing workflows, data integrity, and system integrations are not properly managed. Your EHR touches every aspect of the revenue cycle, including patient data management, insurance verification, charge capture, claim submission, and payment posting. Any disruption in these processes can quickly translate into financial losses.
Common consequences of a poorly executed EHR transition include:
- Billing disruptions and delayed claims, which slow reimbursements and create administrative bottlenecks
- Increased claim denial rates due to coding errors or incomplete documentation
- Data migration errors or loss of critical patient information, risking both compliance and patient safety]
- Workflow inefficiencies across clinical and billing teams, leading to reduced productivity
- Cash flow disruption and revenue loss, impacting the practice’s overall financial stability
Even short-term disruptions can affect accounts receivable (AR) days, collections, and operational performance. The key to a successful EHR switch lies in a strategic transition plan that incorporates data migration safeguards, workflow testing, and comprehensive staff training, ensuring that billing continues smoothly while the practice upgrades its technology.
Why Healthcare Providers Are Upgrading EHR Systems in 2026
In 2026, more US healthcare practices are considering switching EHR systems than ever before. The reasons go beyond just new features; it’s about optimizing workflows, reducing billing disruptions, and supporting patient care while maintaining revenue cycle performance.
Several key factors are driving this trend:
- Outdated Systems and Workflow Inefficiencies
Legacy EHR systems often slow down documentation, charge capture, and billing workflows. These inefficiencies can lead to delayed claims, lost charges, and decreased productivity, putting the practice’s revenue at risk.
- Lack of Interoperability and Integration
Modern healthcare demands EHR systems that seamlessly integrate with labs, clearinghouses, payer portals, and other clinical systems. Without interoperability, data silos emerge, creating billing errors, delayed claims, and AR bottlenecks.
- Revenue Cycle Challenges
Inefficient EHRs directly impact medical billing and RCM, contributing to:
- Missed charges
- Incorrect coding
- Claim submission delays
- Higher denial rates
- Provider Burnout and Documentation Burden
Cumbersome EHR interfaces can increase documentation time, affecting both clinical efficiency and billing accuracy. Staff burnout further amplifies errors, making a seamless EHR migration plan essential.
- Compliance and Reporting Requirements
Regulatory mandates, including HIPAA compliance and reporting standards, require modern EHR systems that support robust auditing, data tracking, and secure storage. Older systems may leave practices exposed to compliance risks and billing penalties.
Key Risks of Switching EHR Systems Without a Billing Strategy
Switching EHR systems or performing an EHR migration is more than just a technical upgrade; it’s a critical operational and financial decision for US healthcare providers. Without proper planning, an EHR transition can disrupt medical billing, increase claim denials, and negatively affect revenue cycle management (RCM). Identifying these risks before starting your EHR system conversion is essential for a smooth, billing-safe transition.
- Delayed Claim Submissions
During an EHR system conversion, workflow disruptions can delay charge capture, claim submissions, and payment posting, impacting your revenue cycle management. Delayed claims increase accounts receivable (AR) days and slow reimbursements, creating cash flow issues. By using parallel billing processes and coordinating EHR migration services, practices can maintain billing continuity. Proper timing and planning reduce billing disruption during the EHR switch and ensure no revenue is lost.
- Coding Errors and Documentation Gaps
Transitioning to a new EHR system can introduce errors in CPT, ICD-10 coding, and documentation if staff are not trained properly. Missing modifiers, incomplete patient encounters, or misaligned EHR workflows can result in claim denials after EHR implementation. This affects reimbursements and adds an administrative burden. Using EHR consulting services, healthcare and testing workflows before going live helps prevent healthcare billing errors and ensures billing workflow optimization.
- EHR Data Migration Errors
An EHR data migration is critical for protecting patient information and ensuring continuity of medical billing. Missing patient demographics, insurance information, or historical billing records can cause claim rejections and RCM disruption. These errors also increase the risk of EHR data loss and HIPAA non-compliance. Partnering with a trusted EHR data migration company or using HIPAA-compliant EHR migration services helps preserve all patient data and reduces potential billing errors in healthcare.
- Payment Posting and Reconciliation Issues
During an EHR transition, payment posting, remittance advice (ERA) processing, and reconciliation can be disrupted, creating gaps in RCM and EHR integration services. Incorrect posting or missing payments can affect financial reporting and revenue collection. Ensuring the EHR implementation company US provides seamless integration with your billing systems helps maintain accurate financial records. Regular monitoring prevents claims processing delays and protects practice revenue.
- Eligibility Verification Failures
Switching EHR systems can temporarily affect real-time insurance eligibility verification, leading to missed or rejected claims. This creates medical billing disruptions, delayed reimbursements, and patient billing confusion. Leveraging healthcare IT consulting EHR and EHR switching support services ensures verification continues uninterrupted. Accurate patient eligibility checks reduce claim denials, protect cash flow, and prevent EHR billing issues.
Pre-Migration Planning: Building a Billing-Safe EHR Transition Strategy
A successful EHR migration begins long before the system is switched. Careful pre-migration planning is essential to prevent billing disruptions during the EHR switch, reduce claim denials, and protect your revenue cycle management (RCM). Without a clear strategy, practices risk EHR billing issues, workflow inefficiencies, and cash flow disruption.
1. Conduct a Revenue Cycle Assessment
Before initiating an EHR system conversion, evaluate your existing medical billing workflows and RCM performance. Review metrics such as:
- Claim denial rates: Identify codes and payers with the highest rejection rates.
- Accounts receivable (AR) days: Determine bottlenecks in claim submissions and payment posting.
- Clean claim rate: Understand how efficiently your current EHR captures charges and processes claims.
- Revenue trends: Track monthly or annual revenue fluctuations to anticipate potential gaps during migration.
This assessment provides a baseline and highlights areas that require workflow optimization during the EHR transition.
2. Audit Billing and Coding Workflows
Review all aspects of your billing processes, including:
- Charge capture and coding accuracy
- Claims submission and follow-ups
- Payment posting and reconciliation
An EHR system conversion will only be smooth if existing inefficiencies are resolved. Address healthcare billing errors and claims processing delays before migration to prevent billing disruption during EHR switch.
3. Identify High-Risk Areas
Some parts of your practice are more vulnerable during an EHR migration. Focus on:
- High-volume procedures: Ensure these are prioritized for accurate billing after transition.
- Frequently denied codes: Pay attention to CPT/ICD codes that often trigger claim denials after EHR implementation.
- Payer-specific requirements: Verify that the new EHR system supports all your payers’ submission rules and formats.
Targeting these areas reduces errors and ensures your EHR switching does not create revenue gaps.
4. Secure Data Backup and Validation
Data is the foundation of EHR system conversion. Before switching systems:
- Create a comprehensive backup of patient records, billing history, and AR data.
- Validate data for accuracy and completeness to avoid EHR data loss risk.
- Work with an EHR data migration company or HIPAA-compliant EHR migration service to ensure secure transfer.
Proper EHR data migration safeguards against claim rejections and protects patient information.
5. Choose the Right EHR Vendor
The choice of vendor significantly impacts your billing continuity and workflow efficiency.
Consider:
- Support for RCM and EHR integration services
- Interoperability with labs, payers, and clearinghouses
- Cloud-based solutions for secure, remote access
- Compliance with US EHR regulations and HIPAA standards
- Availability of EHR consulting services for healthcare to guide implementation
Partnering with a capable vendor minimizes billing errors in healthcare and ensures smooth EHR switching support services.
6. Plan Staff Training and Workflow Adaptation
Your team’s readiness determines the success of the EHR migration:
- Provide hands-on training on billing workflows, coding, and documentation.
- Assign staff roles for monitoring claims processing, payment posting, and RCM performance.
- Use vendor-provided guides, video tutorials, or live sessions to ensure comfort with the new system.
A well-prepared staff reduces EHR transition problems and prevents medical billing disruptions.
Step-by-Step EHR Migration Process Without Disrupting Billing
Successfully switching EHR systems requires a structured approach to protect medical billing, RCM, and claims processing. Following a step-by-step plan minimizes billing errors in healthcare, prevents claim denials after EHR implementation, and ensures a smooth EHR system conversion.
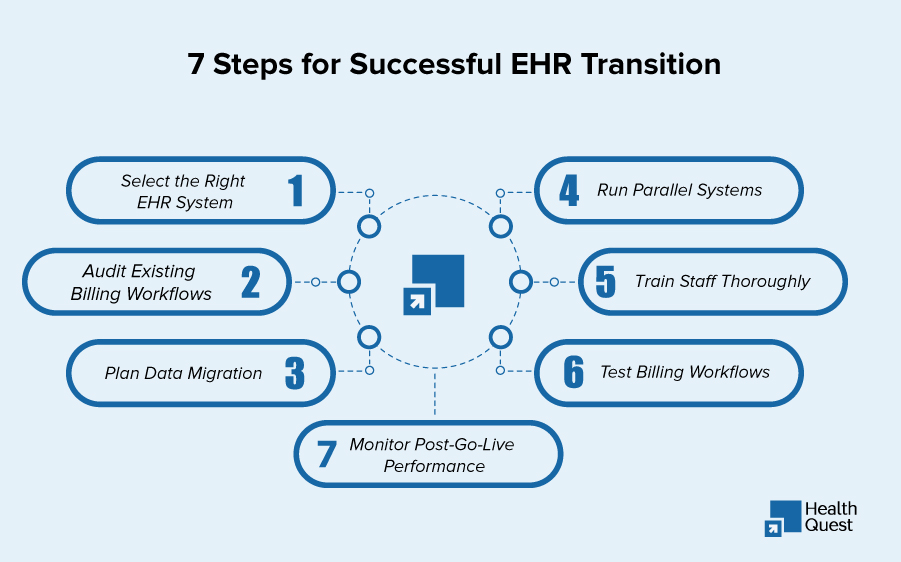
- Select the Right EHR System
Choose an EHR system that aligns with your practice size, specialty, and existing revenue cycle management workflows. Prioritize systems offering EHR implementation services, interoperability with labs and clearinghouses, and HIPAA-compliant EHR migration features. - Audit Existing Billing Workflows
Analyze your current charge capture, coding accuracy, and claims submission processes. Identify potential gaps that could lead to billing disruption during EHR switch. This ensures that the new system accommodates your practice’s RCM and EHR integration services. - Plan Data Migration
Work with an EHR data migration company or EHR consulting services for healthcare to map and transfer patient records, billing history, and insurance information. Accurate EHR data migration prevents healthcare billing errors, claim rejections, and EHR data loss risk. - Run Parallel Systems
Maintain both old and new systems temporarily to avoid cash flow disruption. Parallel operations allow your team to verify eligibility checks, coding, and claim submission without missing revenue opportunities. - Train Staff Thoroughly
Staff should receive targeted EHR switching support services, including hands-on training for charge capture, coding, and patient documentation workflows. Well-trained staff reduces EHR system errors in billing and prevents claims processing delays. - Test Billing Workflows
Before going live, simulate billing cycles for high-volume procedures and payer-specific claim scenarios. This ensures proper RCM and EHR integration and prevents claim denials after EHR implementation. - Monitor Post-Go-Live Performance
After migration, track denial rates, AR days, and cash flow. Implement denial management strategies to resolve errors quickly and ensure accurate claims processing. Continuous monitoring helps optimize EHR workflow efficiency and billing accuracy.
By following these steps, healthcare providers can switch EHR systems without billing disruption, safeguard revenue, and improve operational efficiency while ensuring compliance with US healthcare standards.
Protecting Revenue During EHR Transition
Switching EHR systems without disrupting your revenue cycle can be challenging. US healthcare providers face risks such as billing errors in healthcare, claims processing delays, and insurance claim rejections if proper precautions are not taken. Protecting revenue during EHR migration requires proactive planning, accurate documentation, and workflow optimization.
- Maintain Clean Claim Submission
Accurate coding and documentation are the foundation of preventing medical billing disruptions. Ensure that all charges, CPT/ICD codes, and patient information are correctly transferred to the new system. Mistakes during EHR data migration can result in billing workflow inefficiency and lost reimbursements. Establishing double-check procedures and validating every claim before submission minimizes claim denials after EHR implementation and preserves cash flow.
- Monitor Key Performance Indicators (KPIs)
Tracking performance metrics is essential for safeguarding revenue. Monitor denial rates, AR days, net collection rate, and other RCM indicators to quickly identify issues. By tracking KPIs, you can detect early signs of EHR billing issues, workflow inefficiencies, or EHR system errors in billing. Continuous monitoring ensures corrective actions are applied immediately, preventing revenue leakage and maintaining billing efficiency.
- Use Real-Time Eligibility Verification
Real-time verification of patient insurance eligibility prevents claims processing delays and insurance claim rejections. During EHR transitions, integrating RCM and EHR integration services ensures that eligibility checks are automated and accurate. This step reduces medical billing disruptions and allows staff to focus on claim accuracy rather than chasing missing or incorrect insurance details.
- Implement Denial Management Strategy
Even with thorough preparation, some claims may still be denied. Establish a denial management process that quickly identifies, corrects, and resubmits claims. Partnering with EHR consulting services healthcare or EHR migration services experts can further streamline denial resolution. By proactively managing denied claims, practices prevent billing disruption during EHR switch and protect overall revenue.
- Optimize Billing Workflows
Migrating to a new EHR system provides an opportunity to streamline RCM processes. Redesign workflows to align with the new system, eliminate redundancies, and improve billing workflow optimization. Optimized workflows reduce human error, accelerate claims processing, and ensure billing continuity during the transition. Properly configured systems enhance operational efficiency and safeguard cash flow during EHR system conversion.
- Conduct Post-Migration Audits
Once the new EHR system is live, conduct audits to ensure that all data is migrated correctly and claims are submitted accurately. Verify patient records, billing history, and insurance data to identify any discrepancies. Routine audits prevent EHR billing issues, uncover hidden workflow inefficiencies, and maintain compliance with HIPAA and CMS regulations. Post-migration audits also provide insights for further EHR optimization services.
By combining accurate claim submission, KPI monitoring, real-time eligibility checks, denial management, workflow optimization, and post-migration audits, healthcare providers can protect revenue during the EHR transition. This ensures that switching EHR systems, while complex, does not result in medical billing disruptions, claim denials, or lost cash flow. With the right strategy, EHR migration services can maximize efficiency and maintain financial stability.
Common EHR Migration Mistakes and How to Avoid Them
Switching EHR systems is a complex process, and many US healthcare providers face preventable issues that disrupt medical billing and revenue cycle management (RCM). Understanding these common mistakes can help practices switch EHR systems without billing disruption.
- Inadequate Data Migration Planning
Failing to map and validate patient data, billing history, and insurance details can lead to EHR data loss, claim denials, and billing workflow inefficiencies. Always partner with experienced EHR migration services USA providers to ensure accurate EHR data migration. - Skipping Workflow Documentation
Not documenting current billing, coding, and claims processes increases the risk of EHR-related billing errors. Map your workflows thoroughly to preserve RCM continuity and reduce medical billing disruptions during the transition. - Insufficient Staff Training
Staff unfamiliar with the new EHR system can make errors in claim submission, coding, and documentation. Implement comprehensive EHR switching support services and hands-on training to prevent insurance claim rejections and minimize billing errors in healthcare. - Ignoring Payer Guidelines
Each payer may have specific rules for claim submission and documentation. Overlooking payer-specific requirements can result in claims processing delays and denied claims after EHR implementation. Always review and align your EHR system conversion with payer policies. - Failing to Test the New System
Not running parallel systems or test claims leads to unforeseen EHR billing issues. Conduct pilot testing for high-risk procedures and patient accounts to detect errors early and prevent cash flow disruption in healthcare. - Poor Post-Go-Live Monitoring
After switching, failing to track metrics such as AR days, denial rates, and net collections may cause unnoticed revenue loss. Continuous monitoring allows quick adjustment and supports RCM and EHR integration services for seamless operations.
Avoiding these mistakes ensures your EHR migration is smooth, preserves billing accuracy, and maintains financial stability throughout the transition.
Tips for Smooth EHR Migration (Billing-Safe Transition 2026)
Switching your EHR system without disrupting billing requires meticulous planning and a structured approach. Following a clear checklist ensures your practice avoids medical billing disruptions, claim denials, and RCM workflow inefficiencies.

- Audit Revenue Cycle Management (RCM) performance (denial rates, AR days, claim cycle efficiency) before EHR migration
- Clean and validate patient demographics, insurance eligibility, and clinical documentation to prevent billing errors
- Select an experienced EHR implementation vendor with strong billing integration and EHR migration services
- Run parallel EHR systems to ensure billing continuity and avoid claim submission disruptions
- Train staff on new EHR workflows, medical billing processes, and documentation standards
- Test claims processing, coding accuracy, and payment posting workflows before go-live
- Monitor post-launch RCM KPIs (denial rates, AR days, clean claim rate, reimbursement flow)
- Ensure HIPAA compliance, data security, and accurate healthcare data migration throughout the transition
Need Help With EHR Migration Without Billing Disruption?
Switching EHR systems is a high-stakes decision that directly affects your revenue cycle, claim accuracy, and cash flow stability, where even minor migration errors can trigger denials, delayed reimbursements, and operational disruption. Health Quest Billing helps healthcare providers execute a smooth, billing-focused EHR transition through accurate data migration and validation, aligned billing workflows, denial-prevention strategies, and structured implementation support, ensuring your practice maintains financial stability and uninterrupted reimbursement. Schedule your EHR transition consultation today and protect your revenue from day one.



