Missed rides don’t just frustrate patients; they bleed your practice. U.S. healthcare loses an estimated $150 billion annually to missed appointments, and transportation barriers are a leading contributor. More than 1 in 5 adults without access to a car or transit skipped care in the past year; interventions that remove the transportation barrier measurably reduce no-shows. At the same time, Medicaid requires states to ensure transportation for eligible members, which makes NEMT (non-emergency medical transportation) credentialing a compliance-critical function, not a mere paperwork chore.
What is NEMT Credentialing?
Credentialing for NEMT (non-emergency medical transportation) is the process of verifying if the transportation companies, vehicles, and drivers meet payer, broker, state, and federal requirements so your patients can get to care and your claims get paid. Think of it as three layers:
- Entity/Program Credentialing: Business licenses, insurance, NPI (for some programs), broker enrollment (e.g., MAS in New York), Medicaid/MCO contracts, and compliance attestations.
- Vehicle Credentialing: Insurance limits, inspections, ADA accessibility, lift/ramp documentation, maintenance logs.
- Driver Credentialing: Background checks, motor-vehicle records, drug screens, physicals, CPR/First Aid, PASS/passenger assistance, HIPAA & ADA training; state-specific add-ons (e.g., Florida CPR requirement; Illinois passenger assistance).
The Regulatory Backbone You Can’t Ignore
When it comes to Non-Emergency Medical Transportation (NEMT), compliance isn’t a “nice to have,” it’s a federal and state mandate. Credentialing is the mechanism that ensures providers, drivers, and vehicles meet those mandates, so patients get to care and your organization gets paid.
Medicaid’s Transportation Assurance
Under federal law, state Medicaid programs must ensure transportation for beneficiaries who need it to access covered healthcare services. This isn’t optional; it’s written into the Medicaid statute and further reinforced by the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit. For patients under 21, states are explicitly required to cover medically necessary transportation.
Federal Authority: 42 CFR 440.170 & 42 CFR 431.53
The federal regulatory framework lives in two key provisions:
- 42 CFR 440.170: Defines transportation as a recognized medical assistance service under Medicaid.
- 42 CFR 431.53: Requires states to ensure “necessary transportation” to and from providers is available for all Medicaid beneficiaries.
How states deliver on this requirement varies. Some operate their own transportation programs, others use broker models (like MAS in New York), and many carve transportation out to managed care organizations (MCOs) with their own credentialing rules.
Common NEMT Credentialing Challenges for providers and operators
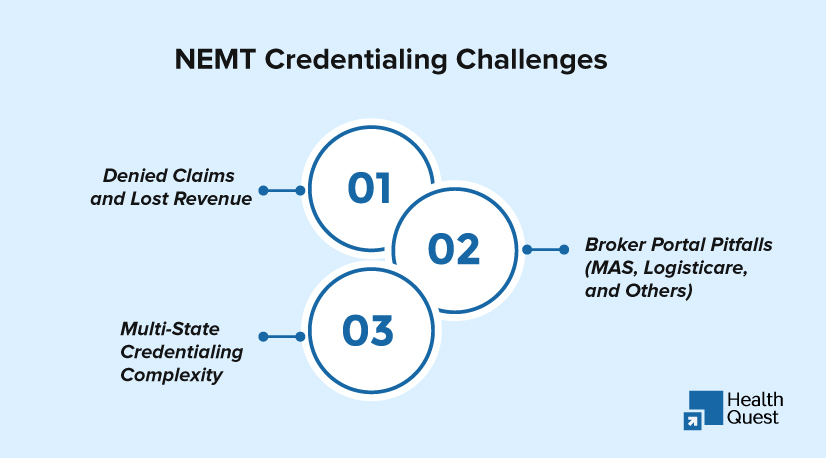
Even though credentialing is the backbone of compliance, many healthcare providers and NEMT operators run into avoidable obstacles that cost time, money, and reputation. These challenges can directly impact revenue cycle performance, Medicaid compliance, and patient care.
Denied Claims and Lost Revenue
One of the most common complaints we hear is about denied NEMT claims. Something as simple as an expired driver certification, a lapsed vehicle inspection, or a missing liability insurance document can lead to payment rejections from Medicaid, MCOs, or brokers. Every denied trip is a missed reimbursement opportunity and a potential compliance flag.
Broker Portal Pitfalls (MAS, Logisticare, and Others)
Providers often struggle with NEMT broker portals like MAS in New York or other national brokers. Common issues include:
- Incomplete or outdated provider profiles
- Mismatched credentials between state Medicaid files and broker systems
- Onboarding delays that hold up new drivers or vehicles
Multi-State Credentialing Complexity
For operators working across multiple states, requirements quickly multiply:
- Different insurance minimums (e.g., $1M in California vs. lower thresholds elsewhere)
- State-specific training mandates (Florida CPR, Illinois passenger assistance, Arizona AHCCCS recertifications)
- Unique revalidation cycles and broker enrollments by state
Key Requirements of NEMT Credentialing Services
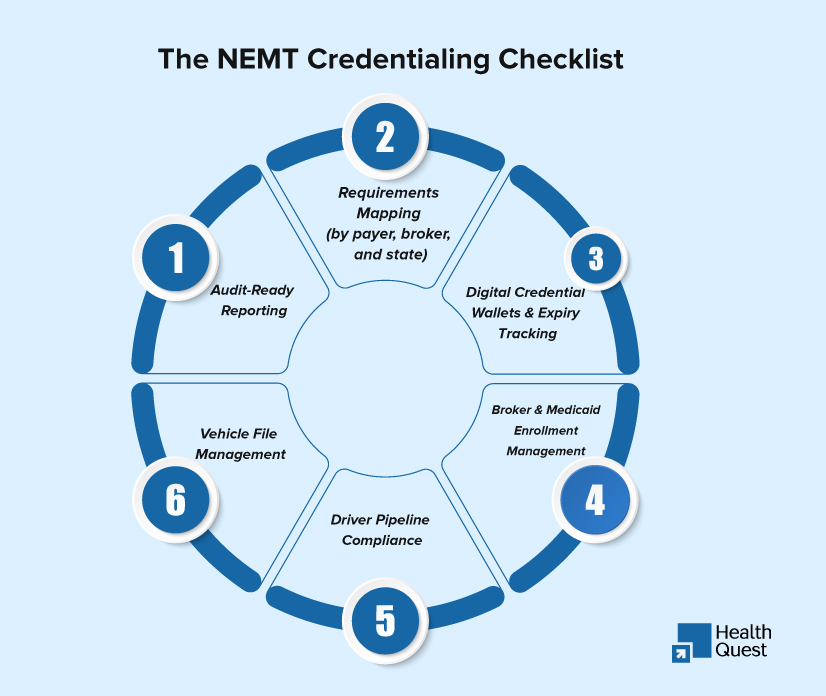
Managing NEMT compliance isn’t about checking a few boxes; it’s about building a sustainable, audit-ready system that keeps trips billable and patients moving. A truly comprehensive credentialing service should address every layer of compliance: the organization, the vehicles, and the drivers.
Requirements Mapping (by payer, broker, and state)
Build a matrix: entity, vehicle, driver; add recert cadence and source citations (statute, broker handbook).
Digital Credential Wallets & Expiry Tracking
Store MVRs, background checks, insurance COIs, ADA/PASS cards, CPR eCards; automate renewal alerts.
Broker & Medicaid Enrollment Management
MAS (NY), state Medicaid portals, MCO rosters submission, revalidation, CAQH/PECOS, where applicable, and change-tracking.
Driver Pipeline Compliance
Pre-hire checklists; standardize CPR/First Aid + PASS; maintain drug screen chains-of-custody and physicals; document ride-type competencies (ambulatory, wheelchair, stretcher).
Vehicle File Management
VIN-level insurance, inspections, lift/ramp certs, maintenance logs, ADA attestations.
Audit-Ready Reporting
Point-in-time credential snapshots, exception reports (expiring/expired), and encounter-date credential proofs.
Key State-Specific NEMT Credentialing Requirements
When it comes to NEMT credentialing, federal rules set the baseline, but the real challenge lies in state-specific and broker-specific requirements. These nuances often catch providers off guard, leading to denied claims, compliance risks, or delayed onboarding.
New York
In New York, the Medical Answering Services (MAS) enrollment process is non-negotiable. Providers must not only complete initial enrollment but also keep profiles updated at all times. MAS periodically revises its credentialing requirements and reporting rules. If providers miss even one update, a driver or vehicle could be suspended until compliance is restored.
Florida
Florida focuses on driver readiness and safety. Every NEMT driver must maintain active CPR certification. If that certification expires, trips may be denied and patients left without transport while providers lose billable revenue.
Illinois
In Illinois, providers are required to ensure drivers complete passenger assistance and safety training. This safeguards patients who rely on wheelchairs, stretchers, or additional mobility support. Failing to meet this standard not only risks claim denials but also increases liability exposure.
Arizona
Arizona’s Medicaid program, AHCCCS (Arizona Health Care Cost Containment System), requires driver and vehicle certification with ongoing recertification cycles. Providers must track these closely; missing a deadline can result in temporary program suspension, blocking access to trips until recertification is complete.
State-Specific NEMT Credentialing Rules
| State | Key Requirement | Risk of Non-Compliance |
| New York | Mandatory MAS enrollment & ongoing profile updates | Suspension of drivers/vehicles; denied trips |
| Florida | Active CPR certification for all drivers | Trip denials, stranded patients, lost reimbursements |
| Illinois | Passenger assistance & safety training | Claim denials; increased liability |
| Arizona | Driver & vehicle certification + mandatory recertification | Program suspension; blocked access to Medicaid trips |
The True Cost of Non-Compliance in NEMT Credentialing
Non-compliance in NEMT credentialing isn’t just a paperwork issue; it directly impacts revenue and patient care. When a driver’s CPR card expires or a vehicle inspection lapses, Medicaid and broker systems can automatically deny claims.
- Per-trip losses: A single denied trip typically represents $40–$150 in lost reimbursement. Multiply that by dozens of rides a week, and the losses add up fast.
- Cascading denials: If credentials are not corrected quickly, denials can continue until the issue is fixed, leading to thousands in lost revenue each month.
- Contract risk: Repeated compliance failures don’t just stop payments; they can trigger audits or even lead to suspension or termination of Medicaid/MCO contracts. Losing one payer contract can wipe out a major share of a provider’s revenue.
- Patient fallout: Beyond dollars, non-compliance leaves patients stranded, dialysis patients miss treatment, seniors skip follow-ups, and trust in your service erodes.

Final Thoughts
NEMT credentialing isn’t just paperwork; it’s how you protect revenue, stay compliant, and keep patients moving. Stay ahead of state and broker rules, and you’ll reduce denials, safeguard contracts, and deliver care without interruption.
Turn Compliance Chaos into Confidence with Health Quest
At Health Quest, we take the complexity out of NEMT credentialing so you can focus on what matters—getting patients to care and keeping your revenue flowing. From managing MAS enrollments and AHCCCS recertifications to tracking driver CPR cards and vehicle inspections, we build a compliance system that works for you, not against you. With our expertise, you’ll avoid denials, pass audits seamlessly, and keep every ride billable.
Ready to streamline your NEMT credentialing? Schedule an appointment with us today.



