Reducing claim denials in medical billing is an important junction for healthcare organizations to manage their finances and patient care. Piled-up claim denials can have a devastating impact on administrative functions and revenue flow.
Therefore, their framework must be intricately dismantled in order to minimize their occurrences. This blog will dissect claim denials and rejections and the steps you can take to overturn their impact.
Also, reduce revenue loss with our claim denials management services. We identify and address denials efficiently, ensuring maximum reimbursement. Discover how we can improve your claim process.
What Are Claim Denials in Medical Billing?
Claim denials are rejections by insurance companies for reimbursement claims filed by healthcare organizations. Insurance companies can deny claims for various reasons, and you must be aware of how to prevent claim denials in medical billing.
You may face a pileup of administrative work or loss in revenue as a result of claim denials. They can have severe implications on the process of medical billing, constraining you from being reimbursed in a timely manner.
What is Claim Rejection?
Insurance companies reject reimbursement claims before processing them. Hospitals usually make one or more errors that lead to claim rejections. Those errors prevent insurance companies from processing those claims.
Your billing and coding staff can make clerical errors. They may enter incorrect details about your patients or medical coding. Also, some information may be missing. Insurance companies scrub claims and reject the ones that have these errors.
Type of Claim Denials
There are two types of claim denials: hard and soft. Insurance companies declare a hard claim denial if they do not cover the services mentioned in reimbursement claims. Your appeals are unlikely to succeed in case of hard claim denials. A soft claim denial is declared due to minor issues.
Insurance companies determine that there are some missing details in reimbursement claims. As a result, they place those claims in review and declare soft denials. This means that soft denials are temporary, and you can reverse them. You just have to make some changes or add the missing details.
Reasons for Claim Denials
Insurance companies can deny reimbursement claims due to various reasons. Such claims may lack the specific criteria for each reason. Let’s see how:
1. Missing Details
Some details can be missing from the reimbursement claims submitted by healthcare providers. A lack of details can result in those claims getting denied by insurance companies. Such details can include modifier information, addresses, and social security numbers.
2. Lack Of Authorization
Hospitals have to authorize their services from the insurance companies of their patients. This has to be done before those services are provided. So, you must conduct this procedure to ensure that insurance companies will pay for your services. Some hospitals do not authorize their services properly and end up with denied claims.
3. Patient Eligibility
Hospitals also have to conduct insurance eligibility verification of their patients. They have to verify whether their patients are eligible to undergo the relevant procedures. It involves checking the insurance plans of those patients. Their plans should cover the medical services they want to avail themselves of. Some claims are also denied if the patients are not eligible for those services.
4. Medical Necessity
Insurance companies also determine if the services provided are medically necessary for patients. They have their own set of criteria to determine that. As a result, they can deny some reimbursement claims if they deem the relevant procedure to be medically unnecessary.
5. Expired Filing Limit
Most of the insurance companies have specific filing limits for hospitals. You must submit your reimbursement claims within their deadlines. Failure to meet those deadlines can get your claims denied by insurance companies.
Steps to Reduce Claim Denials
You can minimize medical billing denials by implementing a multi-faceted and systematic approach to ensure accurate reimbursements for your medical services. Let’s look at some important steps you can take to minimize claim denials and optimize medical billing.
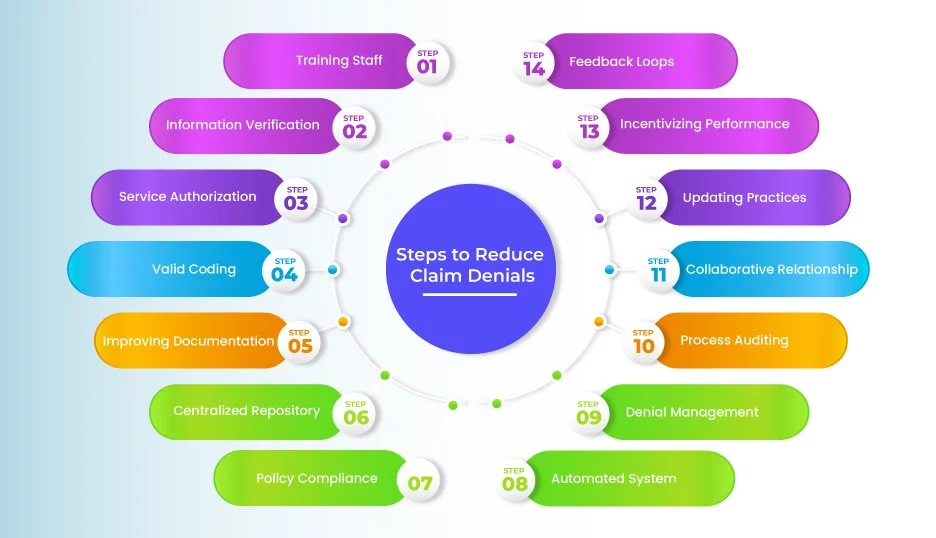
1. Training Staff
You can devise strategies to invest in training and educating your staff. They can be updated with the latest healthcare regulations and guidelines, along with your organization’s insurance policies.
In this way, you can ensure that your staff employees are well-trained to manage patients and their unique circumstances. By doing this, you can prevent technical errors in the documentation that can cause a claim denial.
2. Information Verification
Verification of patient information is also important before reimbursement claims are filed. For claim denials, you must first verify the insurance eligibility and coverage of your patients.
After that, you can qualify them to avail your medical procedures and treatments. With this, updated and accurate patient information can be recorded to prevent denials.
3. Service Authorization
Insurance companies must also authorize your healthcare services by determining whether they are medically necessary for your patients. Your role in this process can include submitting details about your medical treatments and procedures.
They are reviewed by those insurance companies and classified into whether or not they follow the terms and conditions of their policies. You can also contact them to confirm the relevant requirements of service authorization.
4. Valid Coding
Codes assigned to healthcare services also have an impact on the rate of claim denials. You can ensure that correct diagnosis and procedure codes are assigned to their appropriate procedures and treatments.
This increases the chances of appropriate reimbursements claimed for the relevant insurance companies. You can also double-check codes to prevent upcoding and decoding, which assign a higher and lower level code, respectively, to a service.
5. Improving Documentation
You can also work on improving the documentation of your patients to increase their completeness and quality. Details should be complete and thorough enough to support the necessity of your healthcare services.
Sufficient and well-documented supporting information is more likely to justify the eligibility of your patients to avail of treatments and procedures. Subsequently, medical billing denials can be reduced with insurance companies disbursing reimbursements.
6. Centralized Repository
As an additional measure, resources can also be diverted toward creating a centralized repository for the organization and consolidation of information. It can store large sizes of information like insurance coverage, medical records, and personal demographics.
Accumulating patient-related information into a single and accessible repository ensures easy access and appropriate management. At any time, the required data can be retrieved efficiently for the preparation of reimbursement claims.
By doing this, you can minimize claim denials by utilizing accurate information only. This will also be helpful whenever the scale of your healthcare organization grows. A centralized repository can easily accommodate flexible dynamics and handle growing data volumes.
7. Policy Compliance
Policy compliance refers to healthcare organizations like yours adhering to the rules and regulations set by insurance companies. These rules and regulations comprise all policies and guidelines in terms of reimbursement and medical service eligibility.
By complying with their policies, you can increase the likelihood of your reimbursement claims getting accepted. This will improve the process of medical billing as you will be able to generate accurate bills and save the cost arising from non-compliance errors.
8. Automated System
Furthermore, you can automate patient documentation and start working with electronic health records to streamline the process of medical billing. Entire systems like coding can be integrated to ensure an accurate flow of operations.
This leaves no room for human errors as alerts and reminders can be automatically set for important tasks. The rate of missed oversights and deadlines can be significantly reduced if tasks like authorization, filing, and documentation are automated.
9. Denial Management
The claim denial management process incorporates a strategic approach in which reasons for denial claims in medical billing are identified and addressed. The goal is to prevent future denials and resolve existing ones by efficiently managing their reasons.
You can analyze trends and identify patterns in past denials and come up with their root causes. Then, you can use them to implement robust measures and devise corrective actions to prevent claim denials. In this way, you can increase the efficiency of your medical billing.
10. Process Auditing
You must also implement a rigorous auditing mechanism to systematically assess and review all the processes involved in filing medical billing claims. By doing this, you can identify errors, discrepancies, and irregularities at the early stages.
Auditing billing, documentation, and revenue cycles can be beneficial for maintaining efficiency and accuracy in medical billing. Furthermore, you can maintain informative audit trails that can be referenced to draw conclusions and address claim denials.
11. Collaborative Relationship
A collaborative relationship between healthcare organizations and insurance companies is always useful. Both parties can work together to ensure top-notch and stress-free healthcare for their patients and clients.
As a result, potential issues can be swiftly addressed, and the claims process can be effectively managed to prevent claim denials. Any unresolved questions of either party can be resolved by the other party in a timely manner through collaborative communication.
12. Updating Practices
By updating practices, you can compare current processes and outcomes in your healthcare organizations with standardized procedures and benchmark industrial trends. You can also study the relevant successful models to identify aspects of your performance that need improvement.
You can also execute effective strategies to consistently update your practices and minimize denial rates according to industry standards. This enables you to make data-driven decisions and navigate your healthcare organization toward improvements and adjustments.
13. Incentivizing Performance
You can also incentivize the performance of your employees by awarding them bonuses, rewards, and recognition. They can be awarded as a result of their continued dedication and stellar performance, contributing to the increasing growth of your healthcare organization.
Your staff can set performance goals and meet operational targets based on minimizing claim denials and improving the process of medical billing. Simultaneously, you can monitor their metrics to analyze their performance and appropriately provide incentives to motivate them.
It is more likely to motivate them to enhance the quality of filing reimbursement claims and positively drive their professional behaviors. In this way, you can promote financial gains for your organization and as well as elevate the morale of your employees.
14. Feedback Loops
Cultivating an environment where individuals assist each other with feedback is another vital step to reduce medical claim denials. You must encourage a free exchange of insights, opinions, and suggestions between your employees about medical billing and claim denials.
It increases the likelihood of identifying gaps within the system and continuously improving the appropriate responses toward relevant issues. Feedback about any software systems must also be encouraged to decrease technical errors and uphold ideal technology utilization.
All of these actions promote a healthy culture of collaboration and support between your employees. In this way, you can easily highlight their challenges and issues and solve them together to reduce coding denials as much as possible.
What To Do After Receiving A Claim Denial?
You can try appealing after receiving a claim denial if you think it can be reversed. Hospitals regularly submit claim appeals back to insurance companies for further review. This time, you should ensure that your documents are complete and accurate. They must be enough to support your internal appeal.
You should ideally submit an appeal within 3 months of receiving the denial notice. Insurance companies are liable to respond with a written decision. Their decision should be based on a comprehensive review of your appeal. Then, you can investigate their decision and even conduct an external review.
A neutral third party can do that for you if insurance companies continue to deny your claim. However, you must request that they reevaluate their decision before taking this step. They do not have the final say in accepting reimbursement claims after external reviews.
Hospitals can conduct an external review within four months of receiving a claim denial notification. The external review can either agree with the decision of insurance companies. Or it can rule in your favor. Insurance companies must accept whatever conclusion your outside reviewer has reached.
Denial Codes In Medical Billing
Insurance companies use denial codes to represent their claim denials. These codes provide reasons for denying reimbursement claims. You can use those codes to understand the reasons for your claims.
Prepare yourself to appeal the relevant claims denial and resolve your issues. Denial codes are good for insurance companies and patients as they provide transparency. Here are some of the most common denial codes:
1. Claim Adjustment Group Code
Claim Adjustment Group Codes are standardized codes for claim denials. They are specifically used in Electronic Remittance Advice transactions. These codes identify the types and categories of the changes made to reimbursement claims.
These codes include alpha characters. Those characters identify the entity responsible for paying the remaining claim balance. You can use these codes alongside claim adjustment reason codes.
2. Claim Adjustment Reason Code
Claim Adjustment Reason Codes are also used in ERA transactions to justify financial changes. You do not have to assign these standardized codes if there are no changes. In such cases, you have to leave out the CARC column in the Electronic Remittance Advice. You can use these codes to determine any financial changes made to your claims.
3. Remittance Advice Remark Code
These codes provide extra details about the changes given by CARC codes. There are two types of RARCs: supplemental and informational. The supplemental codes do not undergo any distinctions. They provide additional information about claim adjustment reason codes. The informational codes are also called alerts. You can use them to get details about remittance processing.
List Of Denial Codes In Medical Billing
You can save a lot of lost revenue if you understand specific denial codes. We have covered the most common ones for you below:
The Bottom Line
You first need to understand the logic behind claim denials to decide what you can do to reverse them. For that, you have to see how insurance companies work and how they determine whether to accept or deny your claim.
Our professionals at Health Quest Billing offer an expert mix of medical billing services to streamline your revenue cycle. Join us today and become the best at minimizing claim denials and much more.



